Posted May 03rd 2018
Mae’r cynnwys hwn ar gael yn Saesneg yn unig.
These problems can range from anxiety, depression (antenatal and postnatal) and perinatal OCD. Some women can also develop post-traumatic stress disorder (PTSD) if they experience birth trauma. In rarer cases, women can also develop postpartum psychosis, a severe illness that can cause audiovisual hallucinations or delusional beliefs.
If left untreated, these illnesses can have a devastating impact on women and their families. Suicide is a leading cause of maternal deaths in the UK with mental ill-health being a significant factor in many of these cases.
The good news is that with the right treatment and support, women can and do recover.
NICE guidelines outline the standards of service women should receive, and some parts of the UK, women receive world-class care. However, in many parts of the country women have limited access to specialist services resulting in problems going unrecognised, undiagnosed and untreated.
As well as leading to avoidable suffering for women and their families, this is estimated to cost society around £8.1 billion for each one-year cohort of births in the UK.
Maternal mental health is Everyone’s Business
NCMH is part of the Maternal Mental Health Alliance, a coalition of over 60 organisations with a shared vision to see all women get consistent, accessible and quality care and support for their mental health during pregnancy and in the year after giving birth.
Through the Everyone’s Business campaign, the Alliance has played a huge role in raising awareness of the gaps in services, although there is still much to be done. Recently released maps show that pregnant women and new mums in a quarter of the UK still cannot access lifesaving specialist perinatal mental health services, which meet national guidelines.
Momentum in Wales
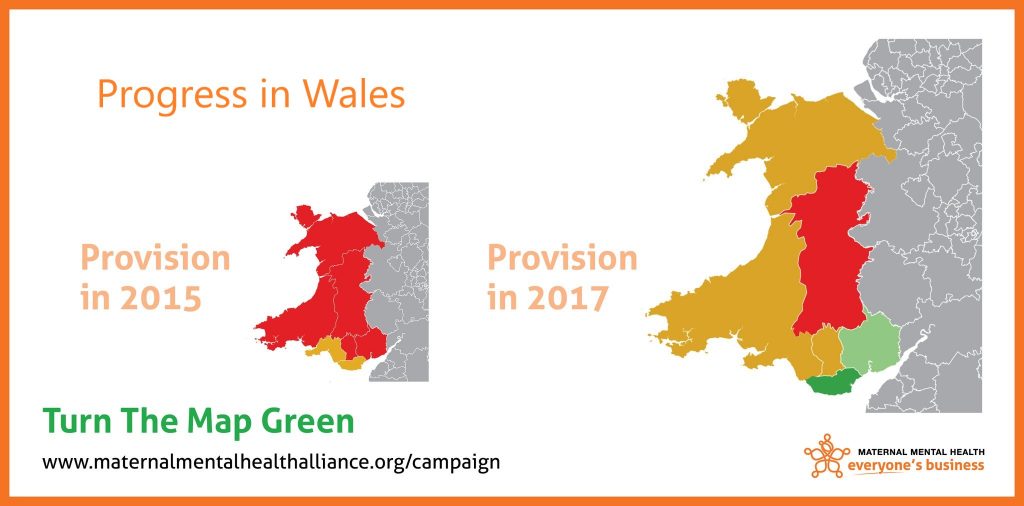
Since the last campaign maps in 2015, there have been improvements in services available to women and their babies.
It’s encouraging to see that Wales has seen the biggest changes, with new and enhanced specialist services in all seven health boards. This is in large part thanks to additional funding of £1.5 million per year from Welsh Government to develop specialist community perinatal mental health services across Wales.
However, this should be seen only as a starting point. There are still a number of issues to address before women and their families in Wales can receive the care and treatment they need. As these maps illustrate, there are still gaps in specialist provision between health boards, and there is a lack of specialist inpatient care (no mother and baby unit) in Wales for women who need it.
The recent report by the National Assembly’s Children, Young People and Education Committee made a series of recommendations to further improve services, many of which were accepted by Welsh Government, has provided a further catalyst for change.
We are building momentum in Wales, and a further report into perinatal mental health provision we’re working on with NSPCC Cymru and partners at Mind Cymru, the Mental Health Foundation will add to the evidence needed to take the next steps and #TurnTheMapGreen.
The report will be launched on Tuesday 12 June at midday in the Pierhead Building, Cardiff Bay. If you would like to join us, there are limited spaces available – contact Publicaffairs.cymru@NSPCC.org.uk to register a space.
Our research
The causes of maternal mental health problems are complex and there is still a lot for us to learn. We are investigating a range of factors that play a role, from genetics and biology to psychology and our environment and life experiences. We hope that by learning more about the causes of these problems we can help develop better treatments and provide support to women at a higher risk of becoming unwell.
